Making sense of COVID-19 vaccine hesitancy in Russia: Lessons from the past and present
August 20, 2021
Share
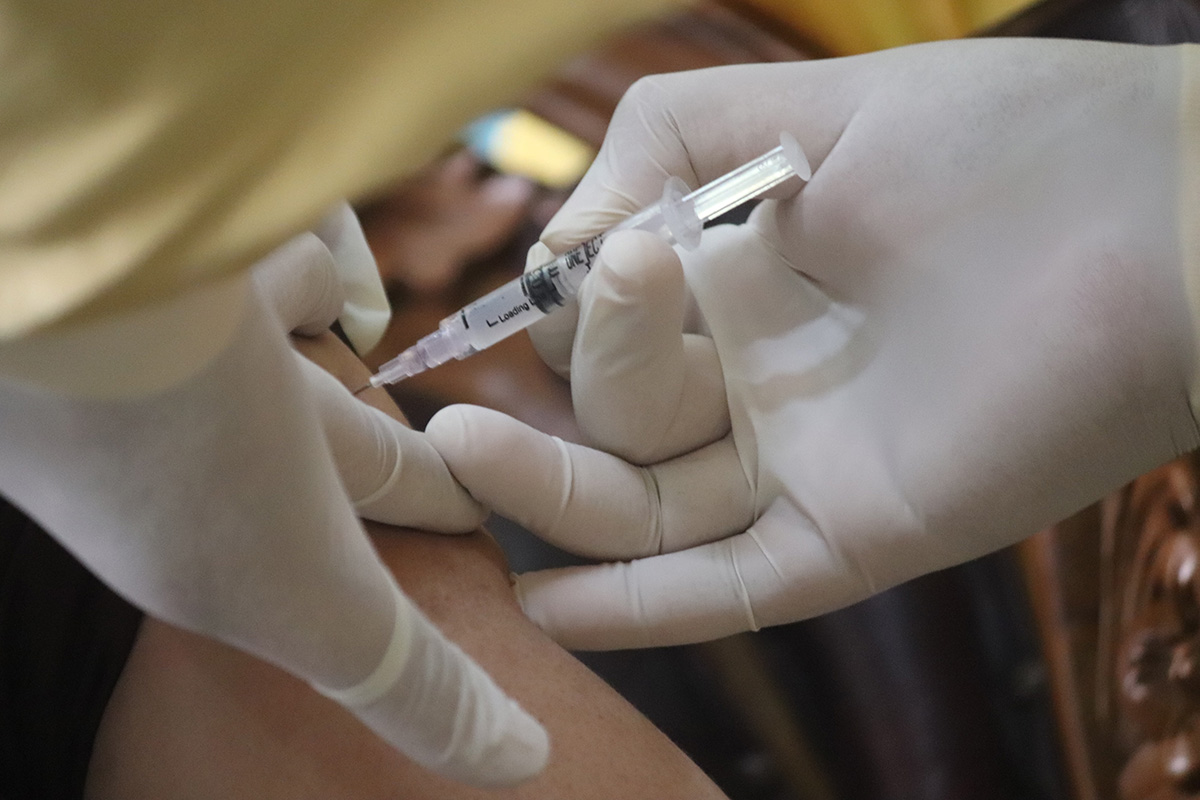
In August 2020, Russia became the first country in the world to approve a COVID-19 vaccine. One year later, just 19 per cent of the population is fully vaccinated. With such a low vaccination rate, a summer surge in infections has produced the highest death rates since the pandemic began. According to official figures, since mid-July close to 800 people have died each day, and these numbers are almost certainly undercounted.
 While other countries have struggled to meet vaccine demand, Russia has faced the opposite problem: an excessive supply, resulting from tepid uptake among a deeply hesitant population.
While other countries have struggled to meet vaccine demand, Russia has faced the opposite problem: an excessive supply, resulting from tepid uptake among a deeply hesitant population.
English-language coverage of the failures of the Russian rollout has focused largely on concerns about safety and ethics protocols in the vaccine development, the prevalence of conspiracy-fuelled vaccine skepticism, inconsistent public health messaging and fear mongering by the media.
Each of these factors plays a part, but Russian-language research (Natalia Mukhina, one of the co-authors, translated the Russian-language research for this article) complicates this picture, highlighting the importance of attending to both the historical roots and contemporary specificities of public health challenges.
From passive subjects to responsibilized consumers
In the former Soviet Union, there was no room for vaccine hesitancy. The national immunization program was massive and mandatory. It was also highly successful, mobilizing domestically produced vaccines to eradicate polio, smallpox, measles and a host of other communicable diseases.
This approach to vaccination started to change in the late 1980s, when the last Soviet leader, Mikhail Gorbachev, launched a series of reforms that would loosen the stranglehold of the authoritarian regime and open a path for the free market.
For the first time in almost seven decades, people were allowed to criticize the Soviet way of life, including the health-care system. Then, during the 1990s, foreign vaccines gradually became available, and new laws required citizens to consent to any medical procedure, including vaccination.
Citizens in what was now post-Soviet Russia went from being passive recipients of state-controlled health-care interventions to responsibilized consumers, who, if they had the necessary resources, could make choices about how to protect their health.
Vaccine skepticism, which was intensifying globally during the 1990s, became one way through which to express resistance to lingering Soviet ideology. But mistrust was rampant across the political spectrum, and vaccine decision making became an arena for the enactment of resistance to the state, even for Russians who believed in vaccines.
Mistrust and marginalization
It is within this context that Russian sociologist Ekaterina Borozdina cautions that public hesitancy about Sputnik, the Russian COVID-19 vaccine, is not “about mistrust in medical science as such.” Rather, hesitation or refusal to get vaccinated emerges in the context of fraught relations between citizens and the state.
In research that predated the pandemic, Borozdina reveals how perceptions of a technocratic, heartless and incompetent government bureaucracy shape the attitudes of Russian parents towards the vaccination of their children.
For educated and economically privileged citizens especially, postponing vaccination, following an alternative schedule, or choosing a particular make of vaccine to be delivered at a particular clinic, are all ways of asserting choice and delineating their independence from the state as they protect what they believe to be the best interests of their children.
Sociologist Anna Temkina further complicates the picture. She says the educated middle classes, a demographic which overlaps significantly with the “activist classes” opposed to the Putin regime, were among the first to get vaccinated, even though they generally try to avoid following government rules and advice. These dissidents make the argument that not everything emerging from the government is bad, and they try to break the link between what they see as a corrupt and oppressive state and effective epidemiological measures.
It may seem surprising that the most enthusiastic consumers of the vaccine are the economically privileged who have the benefit of being able to work from home, but Temkina explains that those who are “indifferent” to vaccines are the couriers or cashiers who worked through the pandemic and “have already overcome COVID-19 or at least the fear of it.”
At the same time, the massive population of migrant workers in Russia who may want protection have largely been denied access — even as Putin offers foreigners the chance to travel to Russia and pay for the vaccine.
Regaining trust
The latest spike in infections has prompted a slight improvement in vaccine uptake, but mistrust is not an easy thing to fix and Russians are once again facing mandatory vaccination as part of an effort to jumpstart the campaign.
This time, the responsibility for enforcement has been offloaded to employers. And employees are finding creative ways to circumvent the new policies. The lengths to which people go to obtain fake vaccination certificates may make for lighthearted news coverage, but wearing a prosthetic limb to a vaccine appointment is an indication of a historical context worth taking seriously if we are to make sense of the challenges ahead.![]()
Samantha King, Professor, Kinesiology and Health Studies,Queen's University and Natalia Mukhina, PhD Student, Kinesiology and Health Studies, Queen's University.
This article is republished from The Conversation under a Creative Commons license. Read the original article.
The Conversation is seeking new academic contributors. Researchers wishing to write articles should contact Melinda Knox, Associate Director, Research Profile and Initiatives, at knoxm@queensu.ca.