Narrowing the gap in health care access
January 14, 2022
Share

When Queen’s researcher Omar Islam (Radiology) first encountered the Hyperfine portable MRI at an international radiology conference in 2019, he immediately realized the potential impact a plug-in magnetic resonance imaging device on wheels could have in remote communities across Canada. Now, thanks to the support of Health Canada and industry partners, Dr. Islam and his team are bringing the portable MRI scanner to Canada’s north for the first time. With patients in these communities having direct access to the device rather than travelling long distances for diagnoses, he and his team will study the potential of this model to serve other sites to help democratize access to health care.
Queen’s and Kingston Health Sciences Centre (KHSC) provide medical services to a predominantly Indigenous population in the Weeneebayko Area Health Authority (WAHA) – Moose Factory and surrounding communities – in Northern Ontario. Currently, patients in WAHA requiring urgent or routine MRI have to be transported by medical charter flight to either Timmins or Kingston. Statistics show that adverse events related to the transportation of critically ill patients can be as high as 60 per cent, with serious incidents occurring in nearly 10 per cent of transports. A portable MRI could reduce these risks by having diagnostic tools directly available to health professionals and the patient.
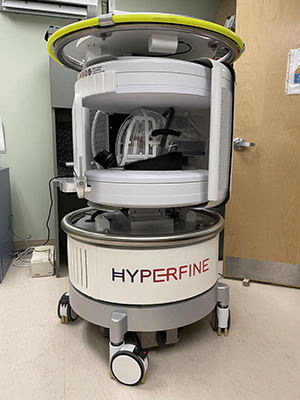
Until very recently, the technology for portable MRIs did not exist. In 2020, a portable MRI device invented by the US-based company Hyperfine received FDA approval and has since been used in academic centers throughout the US and, during the COVID-19 pandemic, in intensive care units for cerebral imaging. The first-of-its-kind device provides imaging for the brain and head in point-of-care settings such as intensive care units, emergency departments, mobile stroke units and resource-limited environments. Unlike traditional machines which can weigh up to three tons, the unit is small enough fit in an elevator and run off a standard power outlet and tablet.
“I thought a portable MRI would be a game-changing technology to bring to Canada, especially in areas where MRI availability is limited or non-existent,” says Dr. Islam. “The analogy would be the introduction of cell phone service to geographically isolated areas around the world where previously even a land-line did not exist.”
Dr. Islam and team have received Health Canada clearance and ethics approval from WAHA and Queen’s for a year-long study on the impact of the portable MRI within the WAHA community. The Hyperfine machine was transported to Weeneebayko General Hospital, in Moose Factory Ontario, where local health practitioners began scanning patients in November.
The team’s study ultimately aims to evaluate the clinical utility and costs savings of a portable MRI in a remote setting such as WAHA. This includes cost-benefit analysis of performing local imaging in comparison to transporting patients to a larger centre. To assess image quality and clinical use, all imaging will be analyzed by board-certified neuroradiologists at KHSC.

Second-year Queen’s medical student, Chloe DesRoche (Right), has been part of this project from early on and was pivotal in assisting with the ethics approvals, communications with Health Canada, organizing logistics with Hyperfine, and training of the health care team in Moose Factory. She is pictured here with Dr. Elaine Innes, Project Co-PI and Chief of Staff at Weeneebayko Area Health Authority. Read more about Chloe's story here.
“We hope to prove that through the availability of a portable MRI to communities in Canada’s north, such as WAHA, there will be improved access to advanced health care, decreased health care costs, and improvement in the lives of patients and their families living in small remote communities throughout Canada,” says Dr. Islam.
Currently, access to MRI scanners is limited by their cost, setting, and infrastructure requirements. The need for neuroimaging can be time sensitive like in cases of an acute stroke, so point-of-care imaging offers the potential for faster diagnosis, treatment, and better patient outcomes.
“The mission and vision of the Weeneebayko Area Health Authority is to provide care as close to home as possible and the Hyperfine MRI project is another big step in that direction. Prior to this, patients in the Weeneebayko region have had to travel south to obtain any MRI imaging so now this eliminates the need for travel, time away from home, etc,” says Dr. Elaine Innes, WAHA’s Chief of Staff. “We are very excited here at WAHA to have one of only two machines in Canada and are very happy to collaborate with Queen’s University and industry partners on this very innovative project.”
Both the Queen’s and WAHA teams hope the findings from this study will guide the use of portable MRIs in other Canadian communities and even around the world.
“This project is a perfect marriage between innovation and delivery of high-quality patient care,” says Dr. Islam. “It serves as a practical example of using technological advances to jumpstart health care innovation for those in our society disadvantaged by lack of access, geographical barriers, and financial constraints. Through this work we hope to help narrow the health care access gap that currently exists between remote communities in Canada’s north and large urban centres.”